1) Information overload but poor understanding
Parents recalled receiving large amounts of information, but still felt that that were not well-informed. This left many parents feeling unqualified for decisional involvement. This indicates that information provision alone is not enough to facilitate decision involvement.
2) Information provision to meet individual needs/preferences
Poor understanding or unmet information needs led many parents to seek additional information, especially online. All parents emphasised the importance of being able to ask questions to their treating team. Being able to ask questions also helped parents feel empowered and part of the decision-making team.
3) Involvement in treatment decisions
Most parents wanted to be involved in major medical decisions for their child. However, many left these decisions to their oncologist because they trusted their oncologist to make the “right” decision, or because they felt they had no choice but to trust. Parents highlighted the benefit of being given opportunities for minor decisions (i.e., decisions that had the same outcome regardless of choice) for both themselves and their child.
4) Decision satisfaction outcome bias
All parents were largely satisfied with their treatment decision, but typically justified this because of the positive outcome of their child’s treatment (e.g. remission). Parents’ decision satisfaction did not appear to be based on the quality of their decision-making process.
Adolescent findings
Due to sample size and difficulty in obtaining in-depth responses, we were unable to conduct a thematic analysis on the adolescent interviews. However, data suggests that adolescents want to be involved in the deliberation of decision, but not necessarily take the lead in determination of the decision.
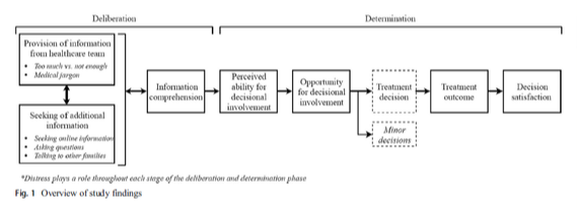
The findings of our study highlight that decision-making in pediatric oncology should focus on involving families in the deliberation phase, rather than just determination of choice. We conclude our study with a modified conceptualization of Elwyn and Miron-Shatz’s decision-making model.
Robertson, E. G., Wakefield, C. E., Shaw, J., Darlington, A. S., McGill, B., Cohn, R. J., & Fardell, J. E. (2019). Decision-making in childhood cancer: parents’ and adolescents’ views and perceptions. Supportive Care in Cancer.
 RSS Feed
RSS Feed